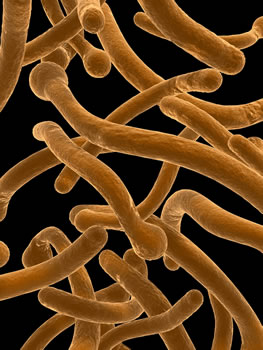
CANDIDA – AN INTRODUCTION
Under normal circumstances there is a carefully controlled balance of yeasts and bacteria within the gastrointestinal tract. In fact, inside our intestines reside approximately 500 different species of micro-organisms, both bacteria and fungi, which act to maintain health. These micro-organisms produce their own antibiotics, thereby maintaining a healthy micro-flora and avoiding the dominance of any single organism. Candida is a yeast, a tiny single celled organism, which is a normal part of the ecology of the skin, digestive tract and vagina. It only becomes a problem when an uncontrolled overgrowth occurs as a result of disruption to the body’s natural immunity and bacterial balance.
Candida is a much used general term. Usually it refers to Candida albicans, yet there are many more species such as Candida parapsilosis or glabrata. Sometimes symptoms can also be caused by moulds like Aspergillus niger or Geotrichum. Once Candida or other fungi have successfully managed to outgrow our healthy intestinal flora, they usually change from harmless round cells into filament shapes which allow them to develop the ability to attach to the intestinal walls making them extremely strong and persistent.
A very important part of our immune system is found within the gut. It is from here that our white blood cells migrate to many other parts of the body. Any fungal overgrowth within the intestines can therefore dramatically affect this process and may cause the immune system to react to a growing number of substances, especially food. This irritation may cause the junctions between the gut wall cells to become more permeable (also know as ‘Leaky Gut Syndrome’), enabling undigested food molecules to enter into the blood stream with the potential to trigger allergic reaction.
SIGNS & SYMPTOMS OF CANDIDIASIS
- Oral or vaginal thrush
- Heavy bloating & flatulence
- Rectal itching
- Depression & mood swings
- Fatigue
- Headaches
- Skin complaints
- Food allergies & intolerances
- Fungal nail infections & athletes foot
- Weight problems
- Cystitis
Even if you think you clearly recognise your own problems within this description, Candida may not in fact be the cause at all. These symptoms may be caused by something completely unrelated so it is important to obtain a safe and accurate diagnosis. There are several laboratories which test for Candida via stool analysis or blood sample.
HOW DOES IT BECOME SO PROLIFIC?
There are several factors, which enable the proliferation of Candida:
- Frequent use of steroidal medications and antibiotics depress levels of beneficial bacteria
- Oral contraceptives induce hormonal changes which can increase Candida levels
- Diets high in nutrients on which yeasts thrive (sugar and refined, simple carbohydrates) provide a constant food source which enables Candida to grow
- A compromised immune system allows opportunistic organisms to flourish
- Endocrine imbalances such as low thyroid and adrenal function, perhaps as a result of stress and blood sugar imbalances, can support the growth of Candida.
CAN DIET ALONE KILL CANDIDA?
If you suffer from Candida, it may mean that your immune system is compromised or your body has been weakened by stress or chronic illness. The traditional anti-Candida diet is incredibly restrictive and for the average person, can be extremely difficult to sustain in the long run. As Candida feeds on sugar and carbohydrates, the elimination of these foods from the diet will certainly help to reduce the number of cells, but in many cases it will not stop the fungi’s ability to cling to the intestinal walls. When Candida is starved of these food sources, the yeast is forced into its cyst form and it will use its fungal ability to lay dormant and rest. In this form it can survive for years and when these food sources are then re-introduced the yeast spores will start to replicate once again. When conditions are favourable for fungi, they can in fact switch to protein digestion anyway, leaving us with an impossible dietary challenge! It would therefore appear far better to maintain the Candida in a weakened and growing form rather than forcing it to lay dormant as this will enable anti-microbial therapies to work to their full potential.
DIETARY DOS AND DON’TS
- Completely eliminate all sugar, sweets, chocolate, fizzy drinks, cakes, biscuits, ice-cream, fruit juice, banana, white/refined carbohydrates and highly processed foods
- Drink 1.5-2 litres of water daily to maintain hydration and help flush out toxins
- Alcohol is generally not recommended, although theoretically, modest amounts of dry wine or spirits may be tolerated
- Consume liberal amounts of good quality protein foods such as poultry, eggs, pulses, fish, nuts, seeds and hard cheese
- Eat unlimited quantities of low carbohydrate foods including all green vegetables, cauliflower, radishes, aubergine, sprouted beans, artichoke, carrots, peppers, olives, tomatoes, cucumber, onions, leeks and peas
- Include 3 servings of low to moderate glycaemic load fruits such as apples, all berries, cherries, lemons, oranges, pears, plums, apricots, grapefruit, nectarines, and pomegranates. (eating a restricted amount of low GL fruits raises the metabolic rate of the yeast, making it easier to kill with anti-fungal treatments).
- Combine proteins with carbohydrates to slow the release of sugar and balance blood sugar levels.
SOME USEFUL NUTRIENTS TO SUPPORT THE ELIMINATION OF CANDIDA ALBICANS
Anti-fungal Agents
Oregano Oil (Origanum vulgare)
This dried herb contains several constituents such as carvacrol, thymol, and borneol, plus flavonoids, rosmarinic acid, triterpenoids (e.g. ursolic and oleanolic acid), sterols, vitamin A and vitamin C. It is the thymol and carvacrol contents in oregano that are responsible for its antimicrobial and antifungal effects. A test tube study demonstrated that oil of oregano (carvacrol in particular) inhibited the growth of Candida Albicans. As oregano oil is absorbed through the lining of the digestive tract and is transported around the body via the lacteal system, it bypasses the liver and maintains its potency throughout the system making it systemically effective throughout the body i.e. in the mouth, digestive tract, vagina and skin.
Stiles JC, Sparks W, Ronzio RA. The inhibition of Candida albicans by oregano. J Applied Nutr 1995;47:96-102.
Journal Applied Microbiology vol 86 June 1999.
Cinnamon Oil (Cinnamomum zeylanicum)
Various terpenoids found in the volatile oil are believed to account for cinnamon’s effects. Important among these compounds are eugenol and cinnamaldehyde. Both cinnamaldehyde and cinnamon oil vapours have been shown to be potent anti-fungal and anti-bacterial compounds.
Singh HB, Srivastava M, Singh AB, Srivastava AK. Cinnamon bark oil, a potent fungitoxicant against fungi causing respiratory tract mycoses. Allergy 1995;50:995-9
Soliman KM & Badeaa RI, Food chem. Toxicol, 2002, Nov;40(11): 1669-75
Coconut Oil
Some of the fatty acids present in coconut oil have antibacterial, antiviral and immune system-stimulating effects.
Sun CQ, O’Connor CJ, Roberton AM. Antibacterial actions of fatty acids and monoglycerides against Helicobacter pylori. FEMS Immunol Med Microbiol 2003;36-9-17
Ruizin A, Novick RP. Equivalence of lauric acid and glycerol monolaurate as inhibitors of signal transduction in Staphylococcus aureus. J Bacteriol 2000;182:2668-71.
Witcher KJ, Novick RP, Schlievert PM. Modulation of immune cell proliferation by glycerol monolaurate. Clin Diagn Lab Immunol 1996;3:10-3.
Ginger Oil (Zingiber officinale)
The principal components of ginger oil are gingerols and shogaols. These pungent constituents are credited with its anti-fungal action.
Agarwal M et al, BJU Int, Dec 2001;88(9): 868-70.
Rosemary Oil (Rosmarinus officinalis)
The volatile oil, including eucalyptol (cineole), is considered to have potent antibacterial effects.
Huhtanen C. Inhibition of Clostridium botulinum by spice extract and aliphatic alcohols. J Food Project 1980;43:195-6.
Garlic (Allium Staivum)
The anti-microbial properties of garlic have been known for centuries, with alliin and allicin being its two active components. Garlic is selective in its inhibition, so does not exert a negative effect on beneficial probiotic bacteria. It is effective against various bacterial and fungal species, and may have a greater potency than Nystatin; a commonly prescribed anti-fungal medication.
Sandhu KD et al, Mykosen, Dec 1980; 23(12), 691-8.
Prasad G & Sharma VD, Br Vet J, Sep-Oct 1980; 136(5), 448-51.
Grapefruit Seed Extract (Citrus grandis)
Also commonly known as citrus seed extract, this is a liquid derived from the seeds, skin and pulp of the grapefruit with anti-bacterial, anti-fungal and anti-viral properties.
Reagor L, Gusman J, McCoy L, Carino E, Heggers JP. The effectiveness of processed grapefruit-seed extract as an antibacterial agent: I. An in vitro agar assay. J Altern Complement Med. 2002 Jun:8(3):325-32.
Heggers JP, Cottingham J, Gusman J, Reagor L, McCoy L, Carino E, Cox R. Zhao JG. The effectiveness of processed grapefruit-seed extract as an antibacterial agent: II. Mechanism of action and in vitro toxicity. J Altern Complement Med. 2002 Aug;8(4):521.
Cvetnic Z, Vladimir-Knezevic S. Antimicrobial activity of grapefruit seed and pulp ethanolic extract. Acta Pharm.
2004 Sep;54(3):243-5
Caprylic Acid
A short chain fatty acid derived from coconut, which has been shown to help maintain a healthy gut flora by favouring the growth of the lactic acid bacteria. It is effective within the lower digestive tract only.
Pau D’Arco (Tabebuia avellanedae, Tabebuia impestiginosa)
Lapachol and beta-lapachone (known collectively as naphthaquinones) are two primary active compounds in pau d’arco. According to laboratory tests, both have anti-fungal properties showm to be as potent as ketoconazole, a common antifungal drug.
Guiraud P, Steiman R, Compos-Takaki GM, et al. Comparison of antibacterial and antifungal activities of lapachol and beta-lapachone. Planta Med 1994;60:373-4.
Also see: The Science of Probiotics and The Truth about Supplements
